Abstract
Research Article
Premaxillary osteotomy in children with bilateral cleft lip and palate: Skeletal and dental changes
Mireia Aznar Gomez*, Lluisa Tobella Camps and Alejandro Rivera Baró
Published: 16 July, 2020 | Volume 5 - Issue 2 | Pages: 011-016
Purpose: To evaluate changes in children with bilateral cleft lip and palate (BCLP) who premaxillary osteotomy and secondary alveolar bone grafting as compared to children with BCLP who are not indicated for surgery, and to determine variables that differentiate patients who do or do not require osteotomy.
Material and methods: Twenty-four children with BCLP were included in the study: 12 who underwent osteotomy (intervention group) and 12 who had no surgery (control group). Radiographic and model values of the intervention group were compared before (T1) and after (T2) premaxillary osteotomy, and measurements were compared with those from the control group at T1.
Results: Convexity, ANB (point A-nasion-point B), and maxillary depth was more diminished at T2 in children in the intervention group. Point A, anterior nasal spine, and pogonion were retroposed after surgery, and the anterior spine was higher. At T2, the upper incisors were proinclinated and intruded, and overbite was improved.
Models revealed increased intermolar intercanine width as well as intrusion of upper incisor after surgery. Premaxilla and upper molars were more extruded, had a higher total maxillary height and increased extrusion of upper incisor in children who underwent osteotomy.
Conclusion: After surgery, children who undergo surgery have a premaxilla that is more normalized and more level with the occlusal plane, as well as improved dental inclination. Variables that differentiate children who require osteotomy from those who do not include more extrusion and protrusion of the premaxilla, and a greater extrusion of the upper incisors.
Read Full Article HTML DOI: 10.29328/journal.johcs.1001032 Cite this Article Read Full Article PDF
Keywords:
Premaxilla osteotomy; Bilateral cleft lip and palate; Cephalometric analysis
References
- Rajmil L, Rivera A, Tobella L. Tratamiento ortodóncico en niños con malformaciones congénitas craneofaciales. Ministerio de Sanidad Servicios sociales e igualdad y la Agència de Qualitat i Avaluació Sanitàries de Catalunya. 2013.
- López Giménez A. Análisis de las alteraciones oclusales y morfología craneofacial del paciente fisurado: Universidad de Valencia. 2015.
- Koh K, Ki H, Suk Oh T, Man Kwon S, Woo Choi J. Treatment algorithm for bilateral alveolar cleft based on the position of the position of the premaxilla and the width of the alveolar gap. J Plast Reconstr Aesthet Surg 2013; 66: 1212-1218. PubMed: https://www.ncbi.nlm.nih.gov/pubmed/23702194
- Meazzini MC, Lematti L, Mazzolemi F, Rabbiosi D, Bozzetti A, et al. Vertical excess of premaxilla in bilateral cleft lip and palate patients: A protocol for treatment. J Craniofac Surg. 2010; 21: 499-502. PubMed: https://www.ncbi.nlm.nih.gov/pubmed/20489454
- Rolando Prada J, García A, Bermudez L, Rojas N, Martínez M, et al. Reposicionamiento de premaxilla protruida y conservación vascular en pacientes con LPH bilateral. Rev Colombiana de Cirugía Plástica y Reconstructiva. 2013; 19: 11-17.
- Jein-Wein Kiou E, Chen PKT, Huang CS, Chen YR. Orthopedic intrusion of premaxilla with distraction devices before alveolar bone grafting in patients with bilateral cleft lip and palate. Plast Reconstr. Surg. 2004; 113: 818- 826. PubMed: https://pubmed.ncbi.nlm.nih.gov/15108871
- Bittermann GK, de Ruiter AP,Janssen NG, Bittermann AJ, Van der Molen AM, van Es RJ, et al. Management of the premaxilla in the treatment of bilateral cleft of lip and palate: what can the literature tell us? Clin Oral Investig. 2016; 20: 207-217. PubMed: https://www.ncbi.nlm.nih.gov/pubmed/26374747
- Aburezq H, Daskalogiannakis J, Forrest C. Management of the prominent premaxilla in BCLP. Cleft palate-Craniofacial J. 2006; 43: 92-95. PubMed: https://pubmed.ncbi.nlm.nih.gov/16405381/
- Geraedts W, Borstlap J, Groenewoud P, Stoelinga P. Long-term evaluation of BCLP patients after early secondary closure and premaxilla repositioning. Int J Oral Maxillofac Surg. 2007; 36: 788-796. PubMed: https://www.ncbi.nlm.nih.gov/pubmed/17618084
- Scott J, Webb R, Flood T. Premaxillary osteotomy and guided tissue regeneration in secondary bone grafting in children with bilateral cleft lip and palate. Cleft Palate Craniofac J. 2007; 44: 469-475. PubMed: https://www.ncbi.nlm.nih.gov/pubmed/17760480
- Toscano D, Baciliero U, Gracco A, Siciliani G. Long-term stability of alveolar bone grafts in cleft palate patients. Am J Orthod Dentofacial Orthop 2012; 142: 289-299. PubMed: https://pubmed.ncbi.nlm.nih.gov/22920694/
- Parri FJ, Soares-Oliveira M, García Aparicio L, Sancho MA, Sarget R, et al. Fisura labiopalatina bilateral: Experiencia de un centro con abordaje multidisciplinar. Cir Pediatr 2001; 14: 124-126.
- Li W, Liao L, Dai J, Zhong Y, Ren L, et al. Effective retropulsión and centralization of the severely malpositioned premaxilla in patients with bilateral cleft lip and palate: A novel modified presurgical nasoalveolar molding device with retraction screw. J Craniofac Surg 2014; 42: 1903-1908. PubMed: https://www.ncbi.nlm.nih.gov/pubmed/25187377
- Kobayadhi S, Hirakawa T, Fukawa T, Maegawa J. Maxillary growth after maxillary protraction: Appliance in conjunction with presurgical orthopedics, gingivoperiosteoplaty, and Furlow palatoplasty for complete BCLP patients with protruded premaxilla. J Plas Reconstr Aesthet Surg. 2015; 68: 758-763. PubMed: https://www.ncbi.nlm.nih.gov/pubmed/25778874
- Costanza Meazzini. Malformazioni craniofacciali: Coordinamento ortodontico-chirurgico. Ed Martina. 2011.
- Camporesi M, Baccetti T, Marinelli A, Defraia E, Franchi L. Maxillary dental anomalies in children with cleft lip and palate: a controlled study. Int J Paediatr Dent. 2010; 20: 442-450. PubMed: https://www.ncbi.nlm.nih.gov/pubmed/20642471
- Koh KS, Han WY, Jeing WS, Oh TS, Kwon SM, et al. Premaxillary Repositioning in the Severe Form of Bilateral Cleft Lip and Palate. J Craniofac Surg 2016; 27: 1440-1444. PubMed: https://www.ncbi.nlm.nih.gov/pubmed/27300460
- Rubio-Palau J, Prieto-Gundin A, Cazalla AA, et al. Three-dimensional planning in craniomaxillofacial surgery. Ann Maxillofac Surg. 2016; 6: 281–286. PubMed: https://www.ncbi.nlm.nih.gov/pubmed/28299272
- Sierra NE, Ferrer-Fuertes A, Salazar-Perez B, Lee GYC, Martí-Pages C, et al. Surgical Repositioning of the Premaxilla Using a Minimally Invasive Endonasal Approach. Cleft Palate Craniofac J. 2018; 55: 830–836. PubMed: https://pubmed.ncbi.nlm.nih.gov/28140669
Figures:
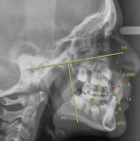
Figure 1
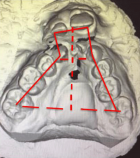
Figure 2
Similar Articles
-
Premaxillary osteotomy in children with bilateral cleft lip and palate: Skeletal and dental changesMireia Aznar Gomez*,Lluisa Tobella Camps,Alejandro Rivera Baró. Premaxillary osteotomy in children with bilateral cleft lip and palate: Skeletal and dental changes. . 2020 doi: 10.29328/journal.johcs.1001032; 5: 011-016
Recently Viewed
-
From Wallets to Waistlines: Exploring the Link between Family Income (Wage Distribution) and Obesity Indices in Pakistani PopulationsAtif Akbar,Waqas Ghulam Hussain*. From Wallets to Waistlines: Exploring the Link between Family Income (Wage Distribution) and Obesity Indices in Pakistani Populations. New Insights Obes Gene Beyond. 2026: doi: 10.29328/journal.niogb.1001024; 10: 001-014
-
Screening for Depressive Symptoms in Clinical and Nonclinical Youth: The Psychometric Properties of the Dutch Children’s Depression Inventory-2 (CDI-2)Denise HM Bodden*,Yvonne Stikkelbroek,Daan Creemers,Sanne PA Rasing,Elien De Caluwe,Caroline Braet. Screening for Depressive Symptoms in Clinical and Nonclinical Youth: The Psychometric Properties of the Dutch Children’s Depression Inventory-2 (CDI-2). Insights Depress Anxiety. 2025: doi: 10.29328/journal.ida.1001047; 9: 028-039
-
Knowledge, Attitude, and Practice of Healthcare Workers in Ekiti State, Nigeria on Prevention of Cervical CancerAde-Ojo Idowu Pius*, Okunola Temitope Omoladun, Olaogun Dominic Oluwole. Knowledge, Attitude, and Practice of Healthcare Workers in Ekiti State, Nigeria on Prevention of Cervical Cancer. Arch Cancer Sci Ther. 2024: doi: 10.29328/journal.acst.1001038; 8: 001-006
-
Oral Cancer Management is not just Treatment! But also, how early Pre-cancerous Lesions are Diagnosed & Treated!!Suresh Kishanrao*. Oral Cancer Management is not just Treatment! But also, how early Pre-cancerous Lesions are Diagnosed & Treated!!. Arch Cancer Sci Ther. 2024: doi: 10.29328/journal.acst.1001039; 8: 007-012
-
Breast Cancer in FemaleLorena Menditto*. Breast Cancer in Female. Arch Cancer Sci Ther. 2024: doi: 10.29328/journal.acst.1001040; 8: 013-018
Most Viewed
-
Physical Performance in the Overweight/Obesity Children Evaluation and RehabilitationCristina Popescu, Mircea-Sebastian Șerbănescu, Gigi Calin*, Magdalena Rodica Trăistaru. Physical Performance in the Overweight/Obesity Children Evaluation and Rehabilitation. Ann Clin Endocrinol Metabol. 2024 doi: 10.29328/journal.acem.1001030; 8: 004-012
-
Hypercalcaemic Crisis Associated with Hyperthyroidism: A Rare and Challenging PresentationKarthik Baburaj*, Priya Thottiyil Nair, Abeed Hussain, Vimal MV. Hypercalcaemic Crisis Associated with Hyperthyroidism: A Rare and Challenging Presentation. Ann Clin Endocrinol Metabol. 2024 doi: 10.29328/journal.acem.1001029; 8: 001-003
-
Effects of dietary supplementation on progression to type 2 diabetes in subjects with prediabetes: a single center randomized double-blind placebo-controlled trialSathit Niramitmahapanya*,Preeyapat Chattieng,Tiersidh Nasomphan,Korbtham Sathirakul. Effects of dietary supplementation on progression to type 2 diabetes in subjects with prediabetes: a single center randomized double-blind placebo-controlled trial. Ann Clin Endocrinol Metabol. 2023 doi: 10.29328/journal.acem.1001026; 7: 00-007
-
Exceptional cancer responders: A zone-to-goDaniel Gandia,Cecilia Suárez*. Exceptional cancer responders: A zone-to-go. Arch Cancer Sci Ther. 2023 doi: 10.29328/journal.acst.1001033; 7: 001-002
-
Ectopic adrenal tissue at the spermatic cordAbdallah Chaachou,Nizar Cherni,Wael Ferjaoui*,Mohamed Dridi,Samir Ghozzi. Ectopic adrenal tissue at the spermatic cord. J Clin Med Exp Images. 2022 doi: 10.29328/journal.jcmei.1001024; 6: 001-002

If you are already a member of our network and need to keep track of any developments regarding a question you have already submitted, click "take me to my Query."