More Information
Submitted: October 31, 2022 | Approved: November 10, 2022 | Published: November 11, 2022
How to cite this article: Houcine Y, Yaiche R, Driss M. An unmistakable tumour of the tongue. J Oral Health Craniofac Sci. 2022; 7: 020-021.
DOI: 10.29328/journal.johcs.1001040
Copyright License: © 2022 Houcine Y, et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
An unmistakable tumour of the tongue
Yoldez Houcine1,2*, Rahma Yaiche1,2 and Maha Driss1,2
1Immuno-Cyto-Histology Department, Salah Azaiez Institute, Tunis, Tunisia
2Faculty of Medicine of Tunis, El Manar University, Tunis, Tunisia
*Address for Correspondence: Dr. Yoldez Houcine, MD, Immuno-Cyto-Histology Department, Salah Azaiez Institute, Bab Saadoun, 1006, Tunis, Tunisia, Email: [email protected]
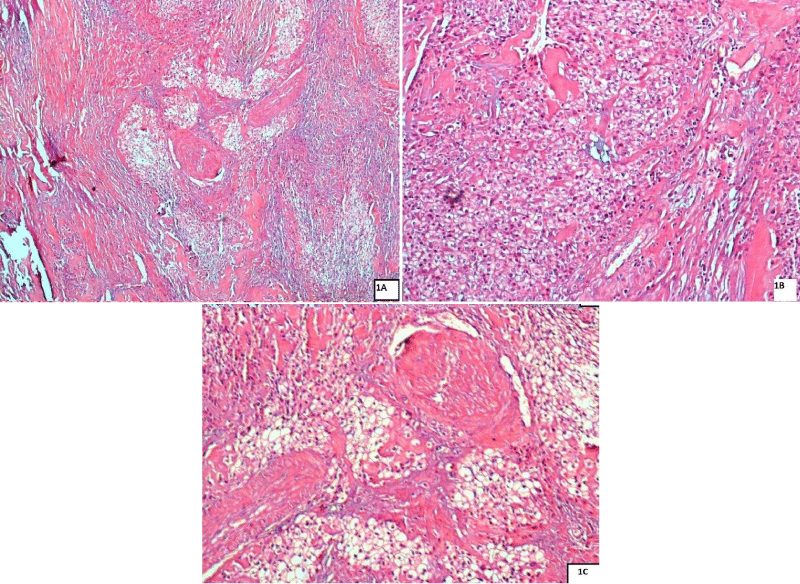
A 37-year-old woman suffered from a painful and swelling lesion of the base of the tongue, with no history of smoking or medical history of tumours. On physical examination, she was found to have an ulcerated and painful induration of the base of the tongue, with no other localization. No cervical adenopathy was found. The CT scan was normal. A Biopsy was done. The exact histological diagnosis couldn’t be done, and pathologists concluded a malignant proliferation. A glossectomy surgical resection was done. The specimen measured 4.5×3×2 cm. The Tumour size was 3×0.5 cm. It was poorly circumscribed and infiltrated the adjacent tissue. The cut surface was greyish-white. The tumour was composed of a monomorphic population of polygonal to round large cells that have optically clear or pale eosinophilic cytoplasm. The nuclei are round and often eccentric, basophilic and sometimes they contain a small nucleolus. Mitotic figures are scars. These tumour cells are arranged in sheets, cords, and nests in a fibrous stroma, with sometimes a scirrhous appearance due to hyalinized collagenous stroma (Figure 1).
Table 1: Mitotic figures are scars.
On immunohistochemistry, tumour cells were positive for P40 and negative for PS100, CD10 and Vimentine.
Question
What is your diagnosis?
Replies
The diagnosis was hyalinized clear cell adenocarcinoma (HCCA) of the minor salivary gland origin.
HCCA is a rare tumor of the salivary gland characterized by myxoid or hyaline degeneration of the stroma arranged in trabeculae, nests, and cords [1]. It can appear in all salivary gland sites with squamous differentiation but mostly presents in the oral cavity at the base of the tongue, palate, or parotid glands [2]. It often metastasizes to locoregional lymph nodes [1,3]. HCCA accounts for only 1% to 2% of all primary salivary gland tumors [4]. Women and men are affected nearly equally [5]. This tumor can be misdiagnosed as mucoepidermoid carcinoma (MEC), epithelial-myoepithelial carcinoma (EMC), and metastases from the kidney of clear cell carcinoma, thyroid, or large bowel can be challenging. Hyalinizing clear cell carcinoma is immunoreactive to p63 and cytokeratins (CK5, CK7, CK8, CK14, and CK19) and negative for calponin, S100 protein, smooth muscle actin (SMA), and glial fibrillary acidic protein (GFAP) [1]. HCCA is most commonly associated with the EWSR1-ATF1 gene fusion. HCCA is typically low-grade and not associated with significant disease-related mortality. Treatment includes primary surgical resection followed by radiation. Data are limited for chemotherapy.
- Weinreb I. Hyalinizing clear cell carcinoma of salivary gland: a review and update. Head Neck Pathol. 2013 Jul;7 Suppl 1(Suppl 1):S20-9. doi: 10.1007/s12105-013-0466-8. Epub 2013 Jul 3. PMID: 23821218; PMCID: PMC3712091.
- Hwang G, Goldenberg D, Warrick J, Slonimsky G. A Hyalinizing Clear Cell Carcinoma of the Base of Tongue. Ear Nose Throat J. 2020 May;99(4):237-238. doi: 10.1177/0145561319840513. Epub 2019 Apr 15. PMID: 30987464.
- Dardick I, Leong I. Clear cell carcinoma: review of its histomorphogenesis and classification as a squamous cell lesion. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009 Sep;108(3):399-405. doi: 10.1016/j.tripleo.2009.03.033. Epub 2009 Jul 1. PMID: 19570692.
- Rodrıguez MS, Reija MFG, Rodilla IG. Primary clear cell carci-noma of parotid gland: case report and review of literature. J Oral Maxillofac Pathol. 2013; 17(1):101-105.
- Daniele L, Nikolarakos D, Keenan J, Schaefer N, Lam A. Clearcell carcinoma, not otherwise specified/hyalinising clear cell carcinoma of the salivary gland: the current nomenclature, clinical / pathological characteristics and management. Crit Rev Oncol Hematol. 2016;102:55-64.